Ultimate Guide for Dental Implant Surgery and Tooth Implant Cost
What is dental implant and what is single tooth implant surgery?
Single dental implants is advanced dental restorations designed to replace a single missing tooth. They consist of three main components: the implant fixture, the abutment, and the crown. The implant fixture is a small, biocompatible titanium screw that is surgically placed into the jawbone, acting as an artificial tooth root. The abutment serves as a connector between the implant fixture and the crown. It is typically made of titanium, zirconia, or another durable material. The crown, which is the visible part of the implant, is custom-made to match the shape, size, and color of the natural teeth.
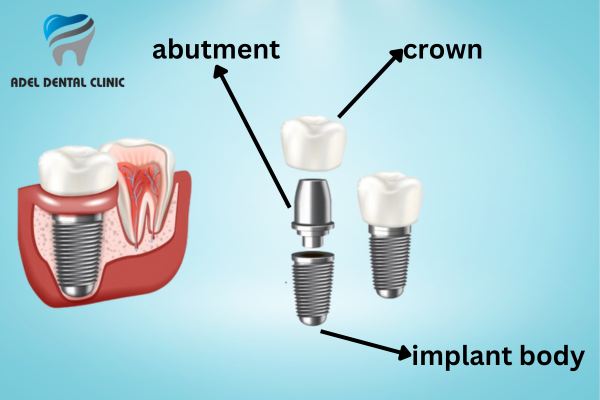
What is the procedure of dental implants?
The procedure for a single dental implant involves several stages. It begins with an initial consultation and examination to evaluate the patient’s oral health and determine the feasibility of implant placement. Following this, a treatment plan is developed based on the patient’s specific needs. In some cases, preparatory procedures like tooth extraction or bone grafting may be required to ensure the implant’s stability and success.
What anesthesia is used for dental implants?
The implant placement surgery is performed under local anesthesia, during which the implant fixture is carefully inserted into the jawbone. After placement, a process called osseointegration takes place, where the bone fuses with the implant over a period of several months, providing a strong and stable foundation. Once osseointegration is complete, the abutment is attached to the implant, and impressions are taken to create a customized crown. The final step involves the placement of the crown onto the abutment, providing a natural-looking and functional tooth restoration.
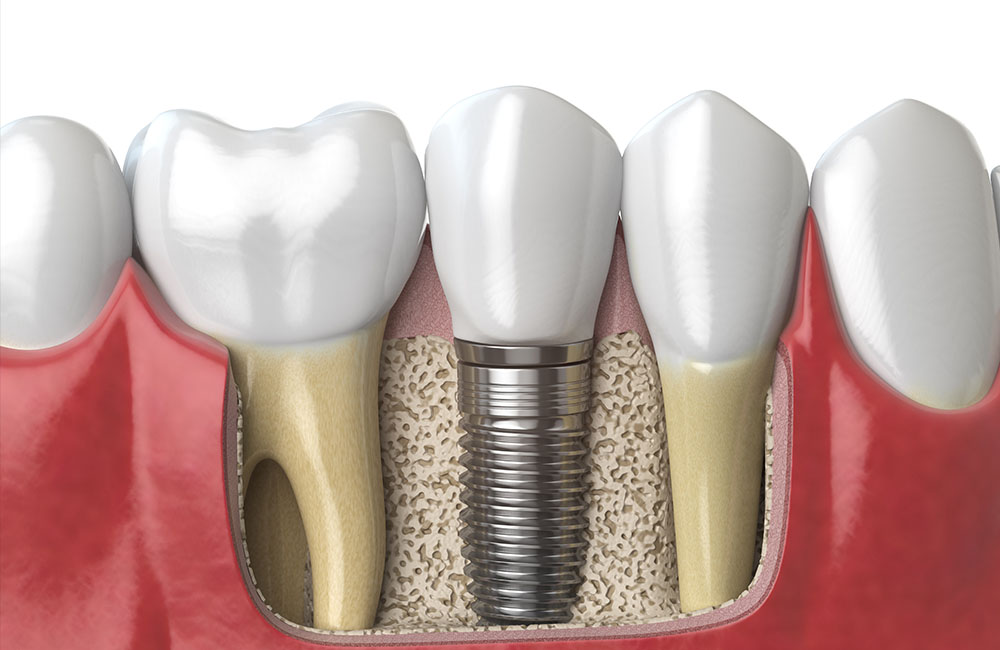
What are the benefits of dental implants
Single dental implants offer numerous benefits, including improved aesthetics, restoration of dental function, preservation of jawbone density, enhanced oral health, and long-term durability. However, as with any surgical procedure, there are potential risks and complications associated with single dental implants, such as surgical risks, infection, implant failure, peri-implantitis, nerve or tissue damage, and allergic reactions.
What is the aftercare for a dental implant?
Aftercare and maintenance are crucial monitör long-term success of single dental implants. Patients are advised to follow post-operative care instructions, practice good oral hygiene, attend regular dental check-ups, adhere to dietary recommendations, and consider lifestyle factors that may impact the implant’s longevity.
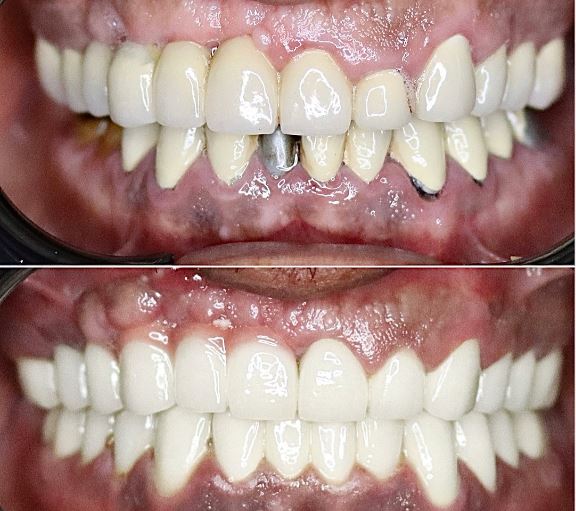
How do you describe a dental implant?
In summary, single dental implants provide a reliable and aesthetically pleasing solution for replacing a single missing tooth. They involve the surgical placement of an implant fixture, followed by osseointegration, attachment of the abutment, and placement of a customized crown. With proper care and maintenance, single dental implants can restore the appearance, function, and confidence of individuals with missing teeth.
What are the advantages of dental implants?
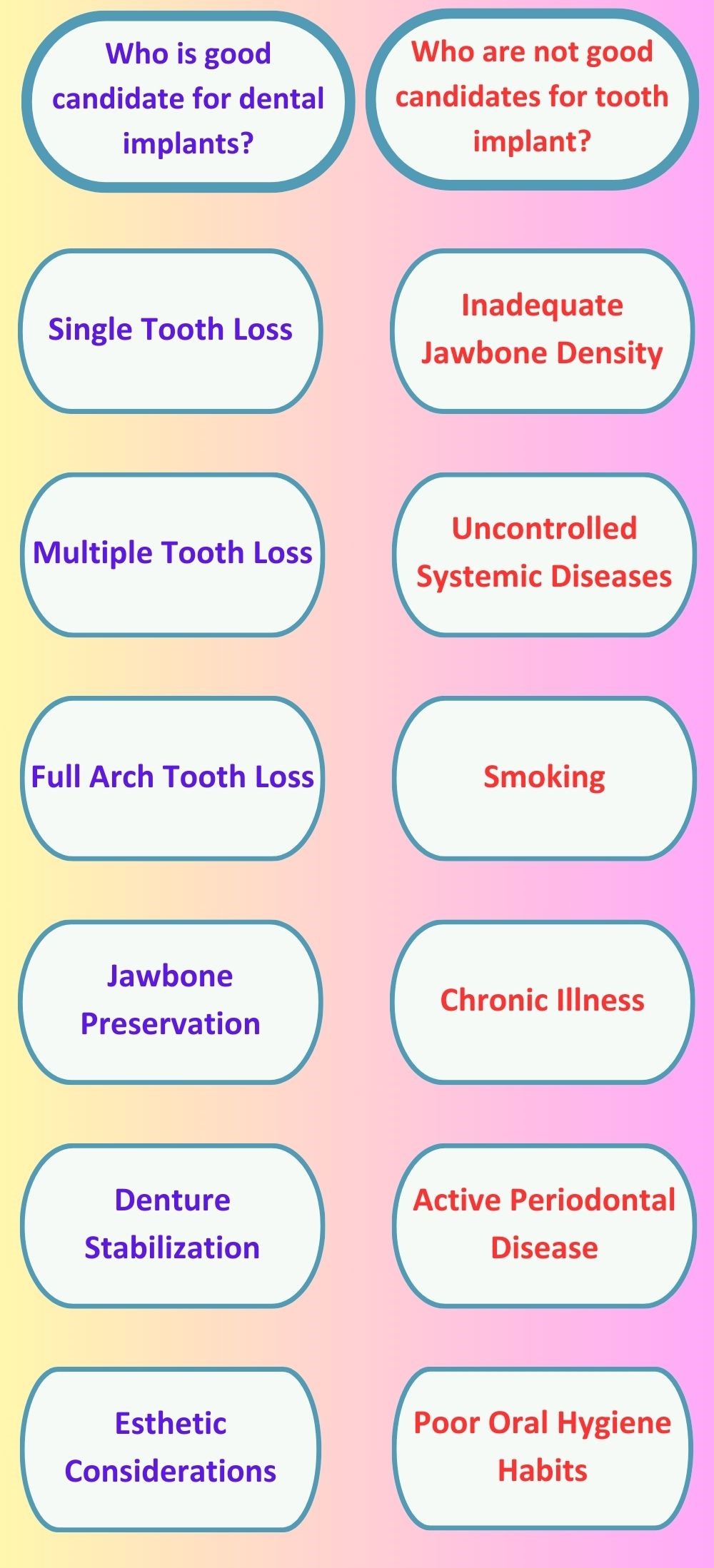
Who is good candidate for dental implants?
- Single Tooth Loss:When a patient has lost a single tooth, a dental implant is often the ideal solution.
- Multiple Tooth Loss:If a patient has lost multiple adjacent teeth, dental implants can be used to support a dental bridge.
- Full Arch Tooth Loss:In cases where a patient has lost all their teeth in either the upper or lower arch, dental implants can be used to support a full arch of fixed implant-supported dentures or an implant-supported overdenture.
- Jawbone Preservation:The titanium implant fixture integrates with the jawbone through a process called osseointegration, which stimulates bone growth and prevents bone loss.
- Denture Stabilization:Patients who struggle with loose or ill-fitting traditional dentures can greatly benefit from dental implants.
- Esthetic Considerations:Dental implants offer exceptional aesthetic results.
Please click here to get more information about "Who is good candidate for dental implants?"
Who is not good candidates for tooth implant?
- Inadequate Jawbone Density:Dental implants require a sufficient amount of healthy jawbone to provide stability and support.
- Systemic Diseases:Certain systemic conditions, such as uncontrolled diabetes or autoimmune disorders, can affect the healing process and increase the risk of implant failure.
- Smoking:Smoking has been shown to impair the healing process and increase the risk of complications, including implant failure.
- Chronic Illness:Some chronic conditions, such as uncontrolled heart disease, liver disease, or immune system disorders, can compromise the body’s ability to heal properly after implant surgery.
- Active Periodontal Disease:Patients with active gum disease (periodontitis) may need to address this condition before considering dental implants
- Age and Growth:Dental implants are generally not recommended for children or adolescents whose jawbones are still growing and developing.
- Poor Oral Hygiene Habits:Maintaining good oral hygiene is crucial for long-term success of dental implants.
Please click here to get more information about "Who is not a good candidate for a tooth implant?"
What should I do before single dental implant surgery?
Before undergoing dental implant surgery, thorough preparation is crucial to ensure a successful outcome. Here is a detailed guide on what to do before dental implant surgery:
- Consultation and Examination: Schedule an initial consultation with a qualified implant dentist to discuss your dental implant treatment. During this visit, the dentist will perform a comprehensive examination, which may include; dental and medical history review, X-rays or 3D imaging
- Treatment Planning and Discussion: Based on the examination results, the implant dentist will create a personalized treatment plan tailored to your specific needs.
- Restorative Options: Explore the different restorative options, such as implant-supported crowns, bridges, or dentures. Consider the advantages, limitations, and costs of each option.
- Costs and Insurance Coverage: Obtain a clear breakdown of the treatment costs and discuss any insurance coverage or financing options available.
- Preparatory Procedures: Depending on your specific case, you may require preparatory procedures before implant placement. These procedures aim to ensure optimal conditions for successful implant surgery. They may include:Tooth Extractions, Bone Grafting, Gum Disease Treatment, Antibiotics Treatment, Stop Smoking, Avoid Eating and Drinking, Recovery Time.
Plase click here to get more information about "What I should do before single dental implant surgery. "
How is dental implant surgery done? in Turkey, Antalya
Dental implant surgery is a multi-step process that involves careful planning, precise execution, and thorough post-operative care. Here are the steps involved in dental implant surgery:
- Initial Consultation and Examination:
Make an appointment for a first consultation with a skilled implant dentist, along with any necessary CT, 3D, or X-ray scans to assess the state of your jawbone, gums, and teeth.
- Treatment Planning and Discussion:
The dentist will make a customized treatment plan that takes into account your unique needs based on the examination and evaluation.
- Preparatory Procedures (if needed):
Teeth may need to be extracted, bone grafting may be done, gum disease treatment may be necessary.
- Implant Placement Surgery:
The dental implants, typically made of titanium, are carefully inserted into the prepared areas. In some cases, temporary abutments may be placed on the implants to shape the gum tissue during the healing process.
- Healing and Osseointegration:
A period of healing is required for implants to integrate with the jawbone. It may take several months to allow the implants to become firmly stable in the bone.
- Abutment Placement and Final Restoration:
The dental implants, typically made of titanium, are carefully inserted into the prepared areas. In some cases, temporary abutments may be placed on the implants to shape the gum tissue during the healing process.
- Post-Operative Care and Follow-Up:
Instructions for maintaining the implants and practicing good oral hygiene will be given by the dentist.
Please click here to get to more info about "how dental implant surgery is done."
FREQUENTLY ASKED QUESTIONS
Is a single dental implant surgery painful?
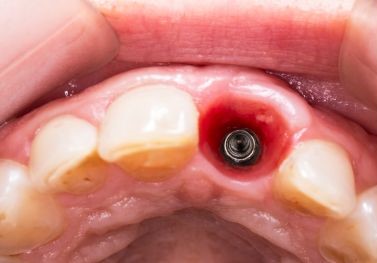
Dental implant surgery is typically performed under local anesthesia, which numbs the specific area being treated. In some cases, additional sedation techniques may be used to help the patient relax during the procedure. Therefore, you feel no pain during the surgery.
After the procedure, some aches could happen, but these can usually be avoided with prescription medicines without being too bothersome.
Please click to get to more info about "Is a single dental implant surgery painful?"
Is it worth it to have dental implant surgery in Turkey?
One well-liked and practical method for improving smile aesthetics and oral functionality is dental implant surgery. A number of significant benefits that Turkey provides are the reason why many patients opt to visit the nation.
- Cost-effectiveness:
The affordability of the treatments is one of the main draws for patients seeking dental implant surgery in Turkey. In general, dental implant procedures in Turkey are less expensive than those in many other nations, including as Europe and the USA.
- High-quality dental care:
Turkey is renowned for upholding high standards of dental care despite the reduced costs. The nation is home to a large number of cutting-edge dental clinics and hospitals that follow worldwide guidelines for patient safety, hygienic practices, and sanitation.
- Experienced and skilled professionals:
Turkey is home to many highly skilled and experienced dental practitioners, including oral surgeons and dentists with a focus on implant dentistry. Many of these specialists are well-known for their skill and accuracy in producing positive results and have a great deal of experience doing dental implant surgery.
- Advanced technology and techniques:
Modern dental implant procedures are made possible by Turkish dental clinics' reputation for investing in cutting-edge dental technologies and methods. Modern diagnostic instruments like cone-beam computed tomography (CBCT) and 3D imaging are among these technological advances.
- Tourism opportunities:
Millions of people visit Antalya Turkey every year. Many patients want to take advantage of the chance to travel and see Turkey's abundant natural beauty by combining their dental implant procedure with a vacation.
- English proficiency:
English is a common language among Turkish dentists, particularly those who treat patients from outside the country. In addition to ensuring efficient communication between patients and their dental care providers, this removes the possibility of language barriers.
Please click here to get to more info about "Is it worth it to have dental implant surgery in Turkey?"
Is Turkey cheaper for dental implant surgery?
In general, dental implant surgery is less expensive in Turkey than it is in many other nations, such as Europe and the US. One of the main reasons patients pick Turkey as their dental implant operation location is the cost advantage. Many patients find that dental implant surgery in Turkey is a financially viable alternative because of the substantial cost reductions that can be realized, even after accounting for travel fees.
How much does dental implant surgery in Turkey?
In Turkey, the typical cost of a single dental implant might be anywhere from $800 and $1500. The crown, or visible portion of the dental replacement, the abutment, which connects the implant to the prosthetic restoration, and the implant insertion procedure are usually included in this price. It is noteworthy to mention that extra expenses can arise based on specific situations, like the requirement for bone grafting or sinus enlargement treatments to guarantee enough bone support for the implant.
Please click here to get more informatin about "How much does dental implant surgery in Turkey?" and "Is Turkey cheaper for dental implant surgery?"What is the success rate of a dental implant?
Dental implants typically have a high success rate; success rates of 90% to 98% have been observed. It's crucial to remember that a number of variables can affect the outcome of dental implants, including the patient's general health, oral hygiene, the implant's location, the type and quantity of bone at the implant site, and the training and experience of the dentist operating on the patient.
The long-term success rates of dental implants have been investigated in a number of studies. The results of these research indicate that success rates are typically quite high. A comprehensive analysis of several studies' findings revealed an overall implant survival percentage of 95.0% after 10 years and 96.4% after five years, according to a systematic review.
What is the most common site for implant failure? Which is a leading cause of dental implant failure?
It's critical to realize that implant failure can still happen and that, as was previously discussed, a number of factors can play a role. However, there is a large increase in the likelihood of a satisfactory outcome with appropriate patient selection, careful planning of the therapy, and strict attention to post-operative care recommendations.
Implant failure can be caused by a number of things. The following are a few typical causes of dental implant failure:
- Poor Osseointegration,
- Insufficient Bone Quality or Quantity,
- Improper Surgical Technique,
- An infection at the implant site can compromise osseointegration,
- Peri-implantitis,
- Poor Oral Hygiene,
- Smoking has been associated with an increased risk of peri-implantitis,
- A number of systemic diseases, such diabetes, can weaken the body's defenses against infection and delay the healing of wounds.
- Overloading;When too much force is applied to an implant too soon, it might cause overloading, which can impede the healing process and result in implant failure.
When is too late for dental implant surgery?
Depending on certain circumstances and factors, there may be a range of acceptable ages for dental implant surgery. Dental implants are a good therapeutic choice for patients of all ages, provided certain conditions are satisfied. It is important to consider the following things prior to dental implant surgery:
- Dental implants are typically best placed once a child or adolescent's bone growth and development are complete.
- There is no minimum age for dental implant surgery because every patient's circumstances are unique.
- Sufficient bone density and quality are required for dental implants to integrate properly.
- For dental implants to be successful over the long term, proper oral hygiene must be maintained.
- The general health of the patient is crucial during dental implant surgery, regardless of age. For instance, immune system issues and uncontrolled diabetes may impede the healing process and increase the risk of complications.
- It's important to take into account the patient's maturity and preparation in this regard.
The choice to have dental implant surgery is ultimately determined by each patient following a comprehensive examination by a qualified dental professional. A number of factors, including patient preparation, age, bone growth, oral health, overall health, and aesthetic concerns, will be considered when determining the ideal time for dental implant insertion.
Please click here to get more informatin about "When is too late for dental implant surgery?"How to heal faster after dental implant surgery?
In order to facilitate quicker healing, recovering following dental implant surgery necessitates appropriate attention and care. Although the duration of recovery may differ for each person, the following basic advice can assist speed up the process:
- Follow Post-Operative Instructions
- Medication,
- Ice Packs,
- Rest and Limit Physical Activity,
- Soft Diet,
- Oral Hygiene,
- Manage Swelling and Discomfort
- Apply Ice Packs,
- Take Pain Medication,
- Avoid Alcohol and Tobacco,
- Maintain Proper Oral Hygiene
- Brushing,
- Flossing,
- Mouth Rinse,
- Eat Nutritious Foods
- Soft Foods,
- Protein-Rich Foods,
- Nutrient-Dense Foods.
Will I be toothless during implant treatment?

You won't be toothless during getting dental implants process. You and your dentist will design a plan of care that will minimise the time you are without teeth while still guaranteeing your comfort and full functionality throughout the process. A few situations that arise during dental implant treatment are as follows:
- Immediate Implant Placement: If simultaneous placement of the implant and tooth extraction is feasible, this method might be employed.
- Temporary Restorations: If your dentist is unable to place an implant right away, they may provide you with a temporary repair to wear while you heal.
- Removable Partial Denture or Bridge: If there are multiple missing teeth in the area where the implants are being placed, you may need to use a temporary solution like a removable partial denture or bridge.
- Existing Denture: You can continue to wear your complete denture after receiving implants if you were doing so previously.
When can I eat after dental implant procedure?
a. Immediate Post-Operative Period (First 24 to 48 hours):
b. Post-Operative Days 2-7:
It is crucial to keep away from meals that can strain the surgical site, such as those that are chewy, crunchy, and firm. Here are some food recommendations for this stage:
c. Post-Operative Days 7 and Beyond:
At this stage, the implant site is getting more stable and the initial healing phase is almost finished. Nonetheless, maintaining a mindful diet is crucial to ensuring appropriate recovery and sustained performance.
Please click here to get more informatin about "When can I eat after dental implant procedure?"Is dental implant surgery combided with other aesthetic treatments?
Combining other aesthetic procedures with dental implant surgery might improve the overall appearance of your smile. Your unique needs and goals, as well as the advice of your dental expert, will determine the precise treatment combination. The following common aesthetic procedures can be used in conjunction with dental implant surgery:
It is crucial to seek advice from a qualified dentist with experience in both aesthetic procedures and implant dentistry. In order to obtain your desired outcomes, they will evaluate your unique needs and offer a thorough treatment plan that combines dental implant surgery with the required aesthetic procedures.
How much does dental implant cost in Turkey?
In Turkey, a single dental implant might cost from $800 to $1500 on average. This usually covers the crown (the component of the replacement tooth that is visible), the abutment (a connector that connects the implant to the prosthetic restoration), and the implant insertion surgery.
Is it worth going to Turkey for dental implants?
Yes, it is worth going to Turkey for dental implants because of;
Additionally, Turkish dental clinics frequently place a high priority on patient education and preventive care in addition to these services. They stress the need of following dental hygiene guidelines, offer dietary advice, and create individualised treatment programmes. Patients in Turkey who avail comprehensive dental treatments are guaranteed to receive personalised and all-encompassing care along their dental journey.

What are the health benefits of dental implants?
Dental Implant Advantages:
What is the best age for dental implants?
Please click here to get more informatin about "What is the best age for dental implants?"
How long do dental implants last?
In order to ensure that the implant teeth last a lifetime, the patient must take good care of their oral and dental health. Furthermore, the longevity of the implant tooth is enhanced by the patient's robust jaw structure and good jaw bone tissue.
For 20 to 30 years, our patients can simply use their implant teeth as long as the required maintenance is taken.
What are the side effects of a tooth implant?
Dental implant-related issues are incredibly uncommon. The primary ones are enumerated here:
Should the implant and jawbone fail to merge, the implant is extracted, and the surface of the bone is cleansed. Approximately three months later, the implants are placed once more.
Is Turkey good for tooth implants?
Yes, Turkey is good for tooth implants because of affordable price/cost-effectiveness, superior dental care, professionals and skilled dentist and comprehensive dental services with cutting edge methods and technologies.
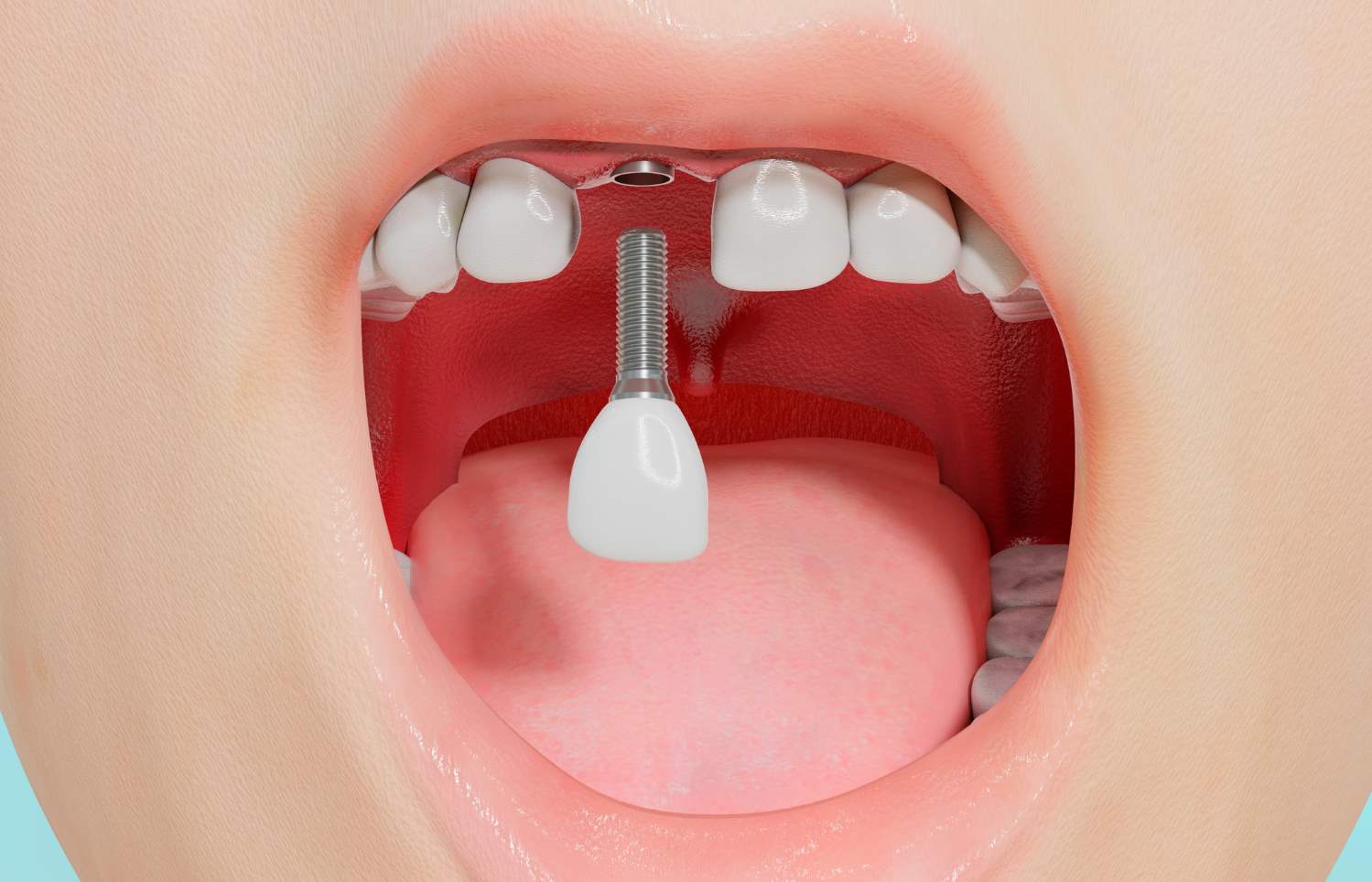
Can you get Turkey teeth with missing teeth?
A dependable and aesthetically beautiful way to replace a single lost tooth is with single dental implant. An implant fixture is surgically inserted, and then the abutment is attached, osseointegration occurs, and a customized crown is placed. Individuals who are missing teeth can have their appearance, function, and confidence restored with single dental implants provided they receive the necessary care and upkeep.
How painful is getting a tooth implant?
For most individuals, receiving implant procedure is just like getting a tooth extracted. Patients don't experience any discomfort because the surgery is done under local anaesthesia. Patients can begin taking painkillers when the anaesthesia wears off, with our dentists' advice.
Which is better bridge or implant?
Choosing implant treatment over a bridge would be a preferable choice given the implant tooth's lifetime, natural appearance, inability to damage neighbouring teeth, restoration of the patient's oral functions, and durability.
It is not necessary to cut and decrease the healthy teeth on either side of the patient's lost tooth and veneer them if an implant is the desired treatment for a single missing tooth. Because of this, implants are crucial for closing tooth gaps without requiring the shrinking or covering of healthy teeth in order to preserve them.
However, because bridge treatment is more cost-effective, it can be recommended.
Are dental implants safe for your health?
In general, dental implants are extremely safe. People with metal sensitivities can use it with ease because of its great biocompatibility. However, in severely allergic bodies, it very seldom causes an allergic reaction.
How much does 1 dental implant cost in Turkey?
A single dental implant might cost between $800 and $1500 in Turkey on average.
Turkey's dentistry offices occasionally provide package discounts or special offers for several implants. Depending on the number of implants needed and the complexity of the situation, the price of multiple dental implants can change. The average cost per implant typically decreases as the number of implants required increases.
Is it a good idea to have dental treatment and to get dental implants in Turkey?
Yes, it is because Turkey is a desirable alternative for people looking for high-quality and reasonably priced dental care because dental implant surgery there is typically less expensive than in many other countries. Before selecting a choice, it's crucial to do extensive research, pick a trustworthy dentist office with qualified staff, and take the entire course of treatment into account.
How long do dental implants last?
With proper maintenance, our patients can comfortably utilize their implant teeth for 25 to 30 years.
How long does implant take in Turkey?
It takes three months for implants placed in the lower jaw and six months for implants produced in the upper jaw for the jawbone to fuse with the implant. Permanent dentures are affixed after the healing and fusing processes are finished.
Where is best to get teeth done in Turkey?
Adel Dental Clinic in Antalya is one of the best places in Turkey. In our clinic, we follow the latest technological developments in oral and dental health and use them in our treatments. Being a health institution that develops and renews itself by complying with scientific and ethical values with our dynamic and innovative physician staff is one of our most important principles. Our aim is to provide quality service by creating accurate diagnosis and treatment plans and to ensure the satisfaction of our patients.
Is it a good idea to have dental treatment in Turkey?
Many patients choose to go to Turkey to have dental treatment because Turkey offers many significant benefits such as sost-effectiveness, high-quality dental care, experienced and skilled professionals, advanced technology and techniques, tourism opportunities and English proficiency.
Why is it so cheap to get your teeth done in Turkey?
The affordability of the treatments is one of the main draws for patients seeking dental implant surgery in Turkey. In general, dental implant procedures in Turkey are less expensive than those in many other nations, including as Europe and the US. There are a number of reasons why dental care is less expensive in Turkey, including better currency rates, fewer labor and overhead costs. Patients can now get the same excellent dental implant surgeries for a lot less money than they would have to pay back in their own nations.
Is there an age limit for dental implant procedures?
For implant treatment, there is no minimum age requirement. The patient must have reached the full growth of their jawbone and have enough width and tissue in their jawbone in order to have implant treatment. The general health status of the patient seeking treatment is sufficient, and there is no maximum age limit for implant treatment.
Do dental implants cause allergies or cancer?
There is no evidence in the research that implants cause cancer. Due to its great biocompatibility, titanium—a material used in many areas of medicine—is used to make implants. Titanium prostheses have long been successfully utilised, particularly in the field of orthopaedics. People with metal sensitivities can utilise it with ease because of its great biocompatibility. In severely allergic bodies, it very seldom causes an allergic reaction.
What is Bone Graft?
Patients with weak and thin jawbones can benefit from bone grafting, which strengthens and expands the bone tissue. Through this procedure, a robust jawbone is prepared for the placement of the implant. There are two methods for obtaining bone graft to be placed in the jawbone: natural and synthetic. While the synthetic bone graft is made from different materials and placed in the jaw, the natural bone graft is implanted using the patient's own bones. The patient's jawbone that has undergone bone grafting requires approximately two months to heal and become implant-ready. The implant surgery begins after the jawbone is ready. Mild bone shortage is seen in the tissue of the jawbone in certain patients. In this instance, the implant and bone transplant operations can be completed by your dentist in the same appointment.
What does a bone graft do in Turkey, Antalya?
If the bone volume is insufficient inside the area where the implant will be positioned, bone graft ought to be applied. Thus, the bone inside the area where the implant can be positioned is bolstered. Bone grafting is also required in sinus lifting surgeries.
What is Sinus Lifting in Antalya, Turkey?
Sinus lifting is a surgical procedure applied during implant treatments on the upper jaw. There are sinus cavities surrounded by the sinus membrane on the right and left sides of the upper jaw. After tooth loss, the sinus membrane moves down. In cases where the patient does not have sufficient bone volume for the implant, the density of the bone is increased by direct or indirect sinus lifting pushing the membrane. This process is called a sinus lifting operation.
What is an immediate load/same day implant in Turkey, Antalya?
It takes several months for implant to integrate with the bone following implant surgery. Nonetheless, early loading can occur without needing to wait for this healing phase in situations where there is enough bone volume. If this operation is right for you, it will be decided by your dentist. With this technique, known as quick loading, the course of treatment can be finished in a few days.
Does the brand of dental implant matter? Which brand of dental implants is the best?
The implant brand used is important in achieving successful results in dental implant treatment. However, the knowledge, experience, and skill of the treating surgeon are inevitable for a successful implant treatment. determines. Generally, world-famous brands such as Straumann, Nobel, and Bio-Tec are preferred by specialist dentists.
Do you need an implant for each tooth?
In patients with more than one missing tooth, dental implants may not be necessary for each missing tooth. Instead, bridge-shaped prostheses can be applied over the implants, depending on the number of missing teeth. For example, in a completely toothless patient, all of the teeth can be replaced by All on 6 treatment.
How many years after tooth extraction can an implant be done?
After the tooth is extracted, the implant can be made if the patient has enough jawbone tissue. Implant treatment may be performed three to six months following tooth extraction if the dentist determines that it is not appropriate to proceed with it on the day of the extraction. Even after a tooth extraction has occurred for a long time, implant treatment can still be performed.
Can implant teeth decay?
The teeth implants do not decay. Since implants are made of artificial materials such as zirconium, titatitanium and porcelain, cavities cannot form in them.
What can be done if an implant fails?
It is possible to retry the unsuccessful implant surgery. The implant must be removed after it has been implanted. The patient receives local anaesthesia. The bone tissue is cleansed once the implant is taken out. Bone grafting is utilised when necessary. One expects the treated tissue to mend. The procedures for creating implant teeth are repeated after the healing phase.
It is possible to install a gingival-like capsule between the implant and the jawbone in situations where the implant does not merge with the bone. The patient may feel pain following this surgery; this is typical.
What happens when your mouth rejects an implant?
The following symptoms may occur; the gums swelling, abrupt allergic response, displacing the implant that was inserted, the patient is in excruciating pain. The implant may not have occurred if the bite and chewing functions are not completely satisfied. You should to make a contact with your dentist.
What happens if an implant hits a nerve?
There is very little chance that an implant will puncture a nerve during treatment. This uncommon circumstance results in the patient losing feeling in the tissues of their lips, jaw, and cheeks.
Is it better to get a bridge or an implant? Which treatment is better?
Healthy teeth on both sides of the missing tooth are decreased for the bridge prosthetic process. After the veneer is ready, the decreased teeth are used as support to create bridges that fill the space left by the missing tooth.
The healthy teeth on either side of the patient's lost tooth do not need to be cut, reduced, or veneered if the implant is the desired treatment for a single missing tooth. Because of this, implants are essential for closing tooth gaps without requiring the shrinking or covering of healthy teeth in order to preserve them.
Gum disease is less likely to occur following implant treatment than it is following bridge treatment. Since bridge treatment is more cost-effective, it is recommended. It would be wiser to choose implant treatment over a bridge, nevertheless, given the implant tooth's longevity, resilience, natural appearance, inability to damage neighbouring teeth, and restoration of the patient's oral functions.
What Are Mini Dental Implants?
Mini Implants are usually used to support a single tooth or a denture and are smaller than standard implants. They might not need as much healing time and can be implanted using a less invasive technique. Compared to standard implants, they can be inserted in a single visit and require less healthy jawbone. For those who have a narrow jawline or little room in their mouth, they can be a decent choice.
Can I smoke and dring alcohol after implant treatment?
There are various reasons that mediate the failure of implant treatment. One of them is smoking and using alcohol. Before starting the implant treatment and after the treatment, it is necessary to quit smoking if possible. If it is not possible to quit smoking completely, it would be appropriate not to use it for a few weeks. Because these habits increase bleeding, delay the healing in the wound area as they decrease the amount of oxygen in the blood. Since it has a negative effect on the immune system, it can also increase the risk of infection.
Is there an age restriction for dental implants?
There is a limit value for the physiological development of each individual. This threshold is generally 18 years old. The physiological development of the jawbone is expected to be completed at this age. It should not be forgotten that there may be young people who have not reached the age of 18, but whose jawbone is developed enough to be implanted. These people can also have implant treatment. The suitability of the person for implant treatment is determined by imaging the teeth and jaws with different imaging devices (x-ray, 3D digital imaging systems, tomography).
What is a seamless implant? When is seamless implant a preferred method?
Seamless implant treatment is preferred by dentists, especially in patients who smoke, because the risk of infection is low. Seamless dental implant treatment is performed with a closed technique. No flaps (incisions) are made on the patient's gums, and this reduces the likelihood of any complications occurring.
In dental implant treatment, the patient's jawbone width must be sufficient for seamless implant treatment. This method can be used if it is determined that your jawbone tissue and width are sufficient in the examinations performed by our experienced dentist before starting the treatment.
Please contact us for more and detailed information
